Menu
- SITCM Overview
- Prospective Students
- Current Students
- Alumni
- Teaching Clinic
The goal of the specialists at the Sydney Institute of Traditional Chinese Medicine (SITCM), is to look for the underlying cause of a patient’s symptoms and treat the individual, not just the disease. The Traditional Chinese Medicine warm (or heat) theory disease is one of the maladies treated at SITCM. This topic is for those who wish to know more about the Chinese Medical procedures that are used to come against these particular infectious agents. The Warm Disease Theory is also called Wen Bing Xue and developed as an independent system during the Qing dynasty.

Warm diseases include disorders such as:
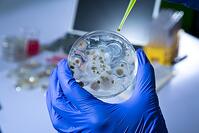
These bacteria and viruses enter the body by way of the nose, mouth, skin wounds, eyes, or any other bodily orifices, so, obviously, the best way to avoid them is to practice careful personal hygiene habits. It was Chinese doctor Ye Tian Shi who developed the idea of using levels to describe the intensities of warm diseases in 220 AD. He labelled the warm disease as having Six Stages. Later, he created the Four Levels which also explained the manner in which these infectious diseases gain entry to the body. Ye Tian Shi found that all these conditions were contagious, included fever, involved a fast development of symptoms, and damaged the patient’s Yin. According to the Miriam-Webster Dictionary, Yin is:
The feminine passive principle in nature that in Chinese cosmology is exhibited in darkness, cold, or wet and that combines with yang to produce all that comes to be.
Level 1 Wei (Defensive)
Wei, in terms of Chinese Medicine, means the immune system, or the first layer of defence. The gastrointestinal tract makes up 80% of this system. When, or if, the disease moves into the circulatory system, fever may occur, along with chills. The collection of signs and methods, called “syndromes” in the Traditional Chinese Medicine (TCM) realm, manifest in warm diseases through:
TCM recommendations that can assist at this level are:
At this level, the disease has taken hold. Symptoms include:
Because the syndrome variations at Qi level are Lung-Heat, Stomach-Heat, Intestines-Dry-Heat, Damp-Heat in the stomach and spleen, and Gallbladder-Heat, the following treatments might help:
Now the disease has almost reached the deepest level. The symptoms at this stage are:
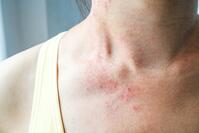
To assuage the symptoms, heat needs to be cooled, blood needs to be tempered, and orifices need to be cleared. Common TCM treatments used at this stage are:

This is the time when the disease has entered the blood and the liver. The kidneys are also involved in this, the final stage of the diseases’ invasion of the body. The symptoms have worsened and take the form of:
In a paper by Qin Bo-Wei, regarded as one of the most prominent physicians, educators, writers, and synthesisers of Chinese medicine of the 20th century, Qin Bo-Wei states:
After one understands the chief patterns, chief signs, and chief formulas of wind warmth then one should combine this knowledge with that of the seasonal aspects of the onset of disease, and other complex factors. Consequently, if one understands all this, even conditions that are complex transformations are not difficult to solve.
The Sydney Institute of Traditional Chinese Medicine (SITCM) is in the business of explaining, teaching, and enlightening lay men and women more about the ancient tradition of Chinese Medicine. Watch for more insights, information, and news and please contact us by clicking in the below.
To book an appointment with the SITCM Teaching Clinic complete your details below.